Metoidioplasty.net » Metoidioplasty Procedures
Vaginectomy: What Trans Men Need to Know

Vaginectomy is a surgery procedure that removes the vaginal lining and closes the vagina. Despite having a a reputation as a risky procedure with high blood loss, Vaginectomy is often combined with Metoidioplasty or Hysterectomy. Many Metoidioplasty surgeons believe that Vaginectomy reduces complications and have made the procedure standard when performing urethral lengthening.
What is Vaginectomy?
In the context of Metoidioplasty, Vaginectomy is a Colpectomy plus a Colpocleisis, but the general term Vaginectomy is more commonly used.
- Colpectomy: Removal of the vaginal lining (epithelium)
- Colpocleisis: Fusion of the vaginal walls, which creates support for pelvic organs.
Some surgeons offer partial closure of the vaginal opening in combination with Simple Release and Ring Metoidioplasty but this is not to be confused with Vaginectomy; it is just a partial closure.
Why Do Trans Men Have a Vaginectomy?
- The desire to have the vagina removed and have a male-looking perineum.
- To eliminate the secretions produced by vaginal mucosa.
- To eliminate the need for speculum exams or Pap tests.
- To reduce complications with Urethroplasty.
How Vaginectomy Is Performed?
- Incisions are made inside the vagina and the vaginal mucosa is carefully removed via excision or abalation.
- The vaginal walls are sutured together and the vaginal opening is closed.
- Operative time is 2-3 hours.
- Laparoscopic and robot-assisted laparoscopic Vaginectomy are emerging methods.
Is Vaginectomy Safe?
There is very little published data regarding the safety of gender-affirming Vaginectomy, but modern techniques Vaginectomy have made the procedure less risky than previously thought. For example, Dr. Burt Webb, one of the most experienced surgeons in the United States when it comes to FTM gynecological surgery, has perfected his Vaginectomy technique to minimize blood loss.
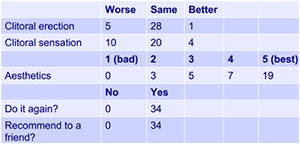
Surgeons at the Institute of Urology London reported that complications with Vaginectomy are few and easy to manage, and that the amount of bleeding is directly related to vaginal length. They also reported a high satisfaction rate among patients.
Can Vaginectomy Reduce Complications with Urethral Lengthening?
Dr. Webb has noted very low rates of complication with urethral lengthening in patients who had Vaginectomy. He believes that eliminating vaginal secretions and improving blood flow to the urethra by fusing the vaginal walls, the urethral junction heals better.
"A normal complication rate when [Vaginectomy] is not done is roughly 40-45% ...the complication rate when a Vaginectomy is performed with these procedures is less than 3%." - Source: ftmdoctor.com
Other surgeons agree:
- Urologist and Plastic Surgeon Dr. Curtis Crane described complication rates of at least 25% when Vaginectomy is not performed alongside Urethroplasty, reducing to 10-20% when it is performed.
- The gender surgery team at VU University medical center, Amsterdam, Netherlands has made Vaginectomy a standard procedure prior to Metoidioplasty with urethral lengthening because they believe it reduces fistula rates.
Because of the theory that Vaginectomy reduces complications associated with the neourethra, some surgeons require a Vaginectomy for patients undergoing Metoidioplasty if Urethroplasty is performed. Hysterectomy is required for all patients having Vaginectomy.
While it is usually performed at the same time as Metoidioplasty or Hysterectomy, Vaginectomy can also be done as a standalone procedure, though Urologist Dr. Maurice Garcia recommends repositioning of the urethral opening to reduce the risk of urinary infections in these cases.
What is Recovery From Vaginectomy Like?
Length of hospital stay, recovery time and time off work all depend on if Vaginectomy was combined with Metoidioplasty or Hysterectomy or done on its own. Some pain is normal but this typically diminishes significantly within two weeks. Restrictions on prolonged sitting, cycling, swimming, hot tubbing, heavy lifting, and sexual activities will also vary based on the procedures done.
Vaginectomy Journal Articles
NEW! Outcomes of Transperineal Gender-Affirming Vaginectomy and Colpocleisis.
Hougen HY, Dugi DD 3rd, Berli JU, Sajadi KP. Female Pelvic Med Reconstr Surg. 2020 Mar 19.
This is a large series studying the outcomes of gender-affirming vaginectomy by complete mucosal excision approach in the literature. Perioperative complications were low: 2 blood transfusions, 1 pelvic hematoma, and 1 C. diff. infection of the colon. No urethral fistulae to the vaginal space, mucoceles, or visceral injures were seen with a median follow-up of 7.7 months. Operative time decreased overtime such that after approximately 20 cases, the procedure fairly consistently takes 2 to 2.5 hours to perform.
NEW! Vaginal Colpectomy in Transgender Men: A Retrospective Cohort Study on Surgical Procedure and Outcomes.
Nikkels C, van Trotsenburg M, Huirne J, Bouman MB, de Leeuw R, van Mello N, Ronkes B, Groenman F. J Sex Med. 2019 Jun;16(6):924-933.
Colpectomy, removal of the vaginal epithelium, may be performed in transgender men because of a disturbed male self-image, to reduce vaginal discharge, or to reduce the risk of fistula formation at the urethral-neourethral junction in future phalloplasty or metaidoioplasty. This single-center retrospective cohort study included 143 transgender men who underwent vaginal colpectomy between January 2006 and April 2018. Vaginal colpectomy is a procedure with a high complication rate, but its advantages seem to outweigh its disadvantages. In all but 1 case, no long-term sequelae were reported. However, the high complication rate and reintervention rate should be discussed with patients who are considering undergoing this procedure.
Colpectomy Significantly Reduces the Risk of Urethral Fistula Formation after Urethral Lengthening in Transgender Men Undergoing Genital Gender Affirming Surgery.
Al-Tamimi, M., Pigot, G. L., van der Sluis, W. B., van de Grift, T. C., Mullender, M. G., Groenman, F., & Bouman, M.-B. The Journal of Urology, December 2018, olume 200, Issue 6, Pages 1315–1322.
A total of 294 transgender men underwent gender affirming surgery with urethral lengthening. A urethral fistula developed in 111 of the 232 patients (48%) without colpectomy and in 13 of the 62 (21%) who underwent primary colpectomy (p <0.01). Secondary colpectomy resulted in 100% fistula closure when performed in 17 patients with recurrent urethral fistula at the proximal urethral anastomosis and the fixed part of the neourethra.
Robot-assisted laparoscopic colpectomy in female-to-male transgender patients; technique and outcomes of a prospective cohort study [Full text]
Freek Groenman, Charlotte Nikkels, Judith Huirne, Mick van Trotsenburg, Hans Trum
Surgical Endoscopy, August 2017, Volume 31, Issue 8, pp 3363–3369.
Study results show that [robot-assisted laparoscopic Vaginectomy] combined with [robot-assisted laparoscopic Hysterectomy] is feasible as a single-step surgical procedure in FtM transgender surgery.
Laparoscopic Vaginal-Assisted Hysterectomy With Complete Vaginectomy for Female-To-Male Genital Reassignment Surgery.
Gomes da Costa, Valentim-Lourenço, Santos-Ribeiro, Carvalho Afonso, Henriques, Ribeirinho, Décio Ferreira. J Minim Invasive Gynecol. 2016 Mar-Apr;23(3):404-9.
This study suggests the feasibility of laparoscopic vaginectomy in genital reassignment surgery. The procedure can be executed as a continuation of the hysterectomy with the potential advantage of the laparoscopy providing better exposure of the anatomic structures with low blood losses (less than 500 mL) and few complications. Furthermore, using this approach, adequate-sized vaginal mucosa flaps were obtained for the urethral reconstruction.
Outcome and Risk Factors for Vaginectomy in Female to Male Transsexuals
M. Spilotros, DJ Ralph, N Christopher, Institute of Urology London, presented at the World Meeting on Sexual Medicine. 2013.
This presentation includes reasons, treatment and results for vaginectomy. Complications are few and easy to manage. The severity of bleeding is directly related to vaginal length. Patients report high satisfaction rates.
Last updated: 03/25/20